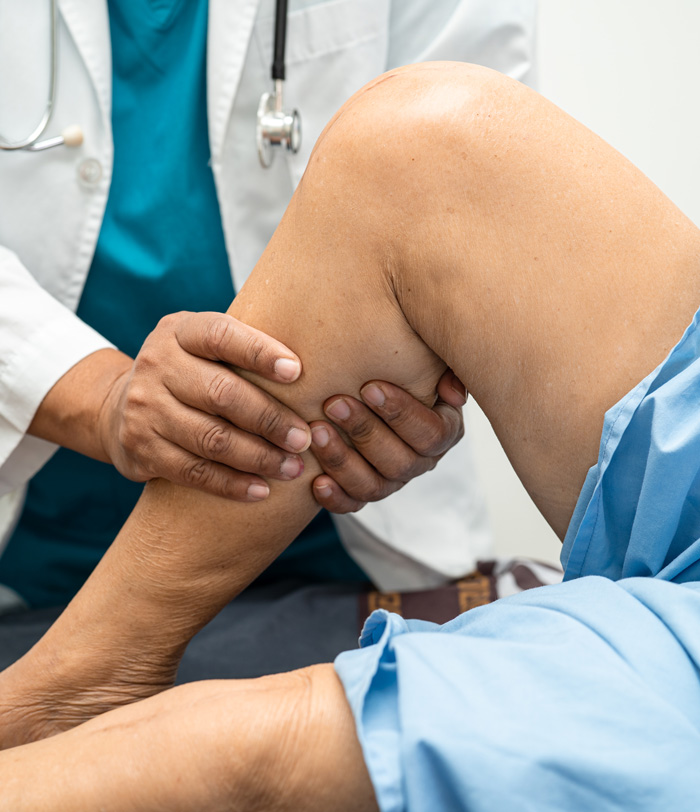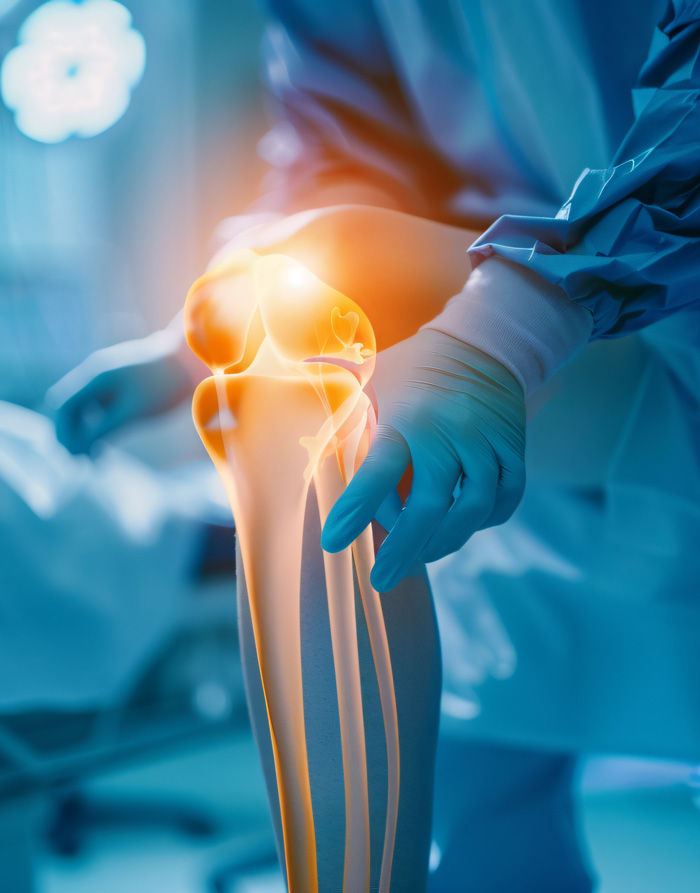
What is knee arthroscopy?
Knee arthroscopy is a minimally invasive surgical procedure carried out through small incisions in the knee and under general anaesthesia. Once you are asleep, a cuff (like a blood pressure cuff) is inflated around the upper thigh to limit bleeding in the knee during the procedure. Through one of the incisions (aka ‘portals’), a thin tube called an arthroscope, which has a small camera and light attached to it, is passed into the knee. Sterile fluid is passed into the knee through another portal to distend the knee and give a clear view. The arthroscope allows me to see directly inside and around your knee joint with magnified images from the camera being transmitted to a screen in the operating theatre.
I can also insert small slender surgical instruments through the other incisions to shave or treat damaged cartilage areas or repair meniscal cartilage. At the end of the procedure, the arthroscope and instruments are withdrawn, the incisions are stitched closed, and dressings are applied.
What is knee arthroscopy used to treat?
Knee arthroscopy is both diagnostic and therapeutic. Leading up to knee arthroscopy, a patient will usually have undergone MRI imaging so we know what we are treating, but it’s only when we can directly visualize the knee at the time of surgery that we can fully appreciate the extent of the problem.
Knee arthroscopy can be used to carry out:
Articular cartilage is the smooth, hard, glistening cartilage that covers the joint surfaces on the end of the femur and the tibia. It doesn’t have the capacity to regenerate if damaged because it doesn’t have a blood supply. Trauma and long-term adverse physical loading can damage the cartilage surface, which can cause pain in the knee, swelling, catching, locking, and stiffness. The articular cartilage consists of layers of cells, collagen, and other molecular structures that sit on top of the surface of the bone known as the subchondral bone plate. This bone has a good blood supply, which can be harnessed during a microfracture procedure.
If the damage to the articular cartilage is more superficial (known as partial thickness damage), the affected area can be smoothed and stabilized using a radiofrequency probe at the time of the arthroscopy. The probe produces electrothermal (radiofrequency) energy which smooths the articular surface and gives it mechanical stability.
If there is more severe or full-thickness cartilage loss within the joint, I may occasionally use a technique called microfracture. Where there are defects in the cartilage (e.g., down to the bone beneath), I smooth off the edges and remove any loose flaps or debris. Using a tiny metal instrument, I knock small holes into the bone plate to create a little bleeding. Because the bleeding comes directly from the bone, it’s rich in natural stem cells with great healing potential. Over time, this clotted blood matures into a scar patch filling the defect. While this scar cartilage can never be as good as the original articular cartilage, it’s better than leaving the bone exposed. Most people can expect excellent results from their microfracture for around five years, and microfracture is suitable for small articular cartilage holes (e.g., less than 2 cm in diameter).