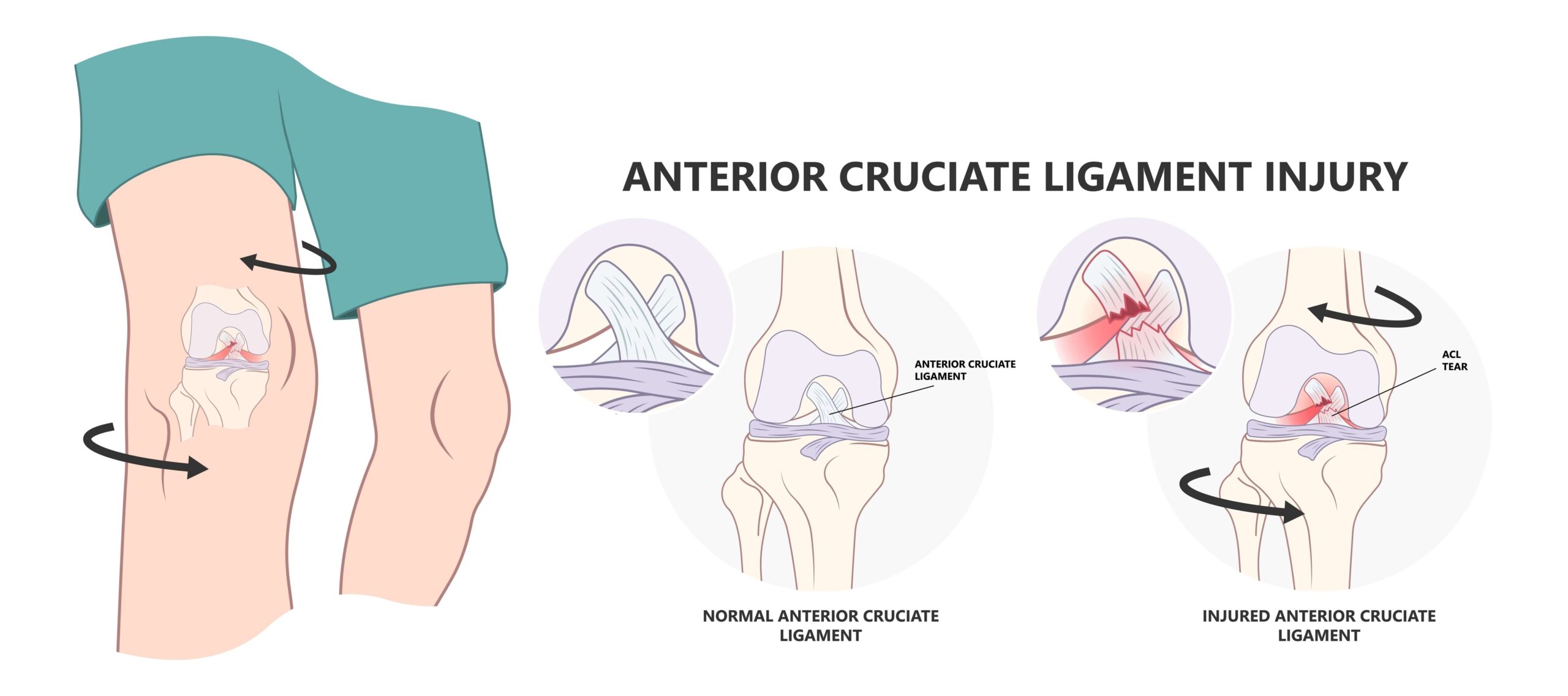
ACL Tear Mechanism
How does an ACL tear occur? When we think of ACL tears, we often think of football, but any sudden pivoting or change-of-direction activity can tear an ACL, as can landing awkwardly after a jump. Sometimes, a tear happens when the knee is struck forcefully from the side.
Some people sense or even hear a ‘pop’ when the ligament tears, and they may fall to the ground or find it very difficult to bear weight. The knee will typically start to swell (because of bleeding into the knee) briskly, and while some people experience pain, others experience little or no pain. Most people, however, will know that something significant has happened to the knee or that the knee feels unstable.
Most ACL tears have an accompanying injury. Around 60% of people who tear their ACL will also have injured a meniscus, but many people will also have tearing of another ligament, such as the medial collateral ligament (MCL), or damage to the articular cartilage lining the joint.
ACL tears are more common in females, and female athletes are 4-5 times more likely to suffer an ACL tear than male athletes. There are many reasons for this, including:
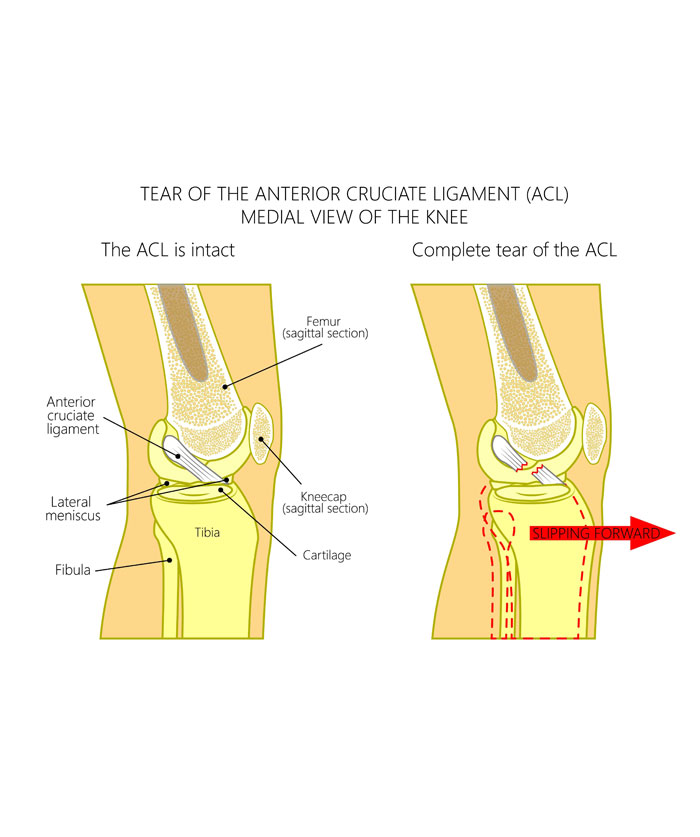
What About Partial ACL Tears?
Many people wonder if a partially torn ACL can repair itself or if it requires surgical repair. Generally speaking, if the knee is stable, then a trial of physio rehabilitation is a good option.
Should I Have ACL Surgery?
ACL reconstruction surgery isn’t for everyone. Many people with low athletic demands on their knees or those who are much older do very well with conservative rehabilitation, such as physio and strength work. I do my very best to help guide my patients through this decision-making process by deeply understanding their needs. The decision is very much a joint decision.
If you regularly play sports that involve jumping or twisting, if your occupation is physically demanding, if your knee regularly gives way, or if other structures in the knee are also damaged, we may decide that ACL reconstruction is for you.










